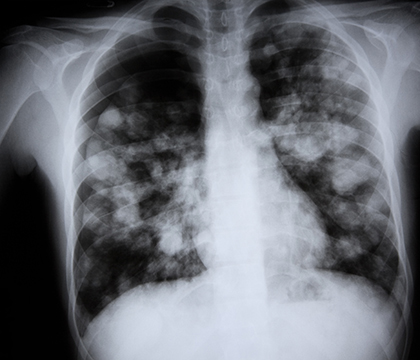
Scientists seek therapies for severe flu cases
A research team at the Western College of Veterinary Medicine (WCVM) is investigating how they can stop severe influenza virus infections from causing a fatal build up of fluid in patients' lungs.
By Taryn Waugh"This research will eventually enable us to treat and overcome severe infections where patients are essentially drowning from the fluid build up in their lungs," explains Dr. Matthew Loewen, assistant professor in WCVM's Department of Veterinary Biomedical Sciences.
Every year, strains of influenza A virus infect millions of people worldwide. These infections annually result in more than 500,000 deaths, and that number is substantially higher when pandemic strains of influenza emerge.
These strains appear because influenza viruses are capable of infecting — and transmitting between — a wide variety of hosts. While people, pigs and birds are the most common hosts, other species can also become infected.
Each strain of influenza virus causes illness in a slightly different manner, and some strains cause more severe disease than others.
"Given that each year a large proportion of the population succumbs to influenza virus infection, it is important to further understand what drives the pathogenesis of this virus," says Loewen.
Typically, the deaths are due to influenza's ability to infect and disrupt the basic cellular mechanisms of epithelial cells that line the host's nasal cavity and trachea (upper respiratory tract).
The epithelial cells form a barrier that separates the air-facing (apical) and blood-facing (basolateral) sides of the cells. This division is important to ensure proper hydration within the airways.
Why is airway hydration so important? It helps to clear out inhaled debris that ultimately gets trapped in the mucus layer lining the airways. This fluid and mucus layer (or airway surface liquid) is maintained by the movement of sodium, potassium and chloride ions through pumps and channels in the epithelial cell membrane.
Potassium exits the cell through ion channels on the air-facing and blood-facing sides of the epithelium, making the electrical charge within the cell more negative. This, in turn, forces chloride through ion channels in the apical (air-facing) cell membrane and into the airways.
The movement of chloride ions creates a gradient for both sodium and water to follow, which results in the correct level of airway hydration.
But when this process is disrupted, it can lead to over- or under-hydration of the airways. Chloride exits the apical membrane either through the cystic fibrosis transmembrane regulator channel or other chloride channels present in the cell membrane.
In the case of influenza virus infection, researchers see increased chloride movement through these channels. The result is over-hydration of the airways that can lead to pulmonary edema. If it isn't corrected, this build up of fluid in the lungs can ultimately cause a patient to drown.
Using a well-established model, the WCVM research team is determining how influenza virus infection modulates ion channel function to cause pulmonary edema.
"Our goal is to identify the direct and indirect effects of influenza virus infection on both chloride and potassium channel function," says Loewen.
Preliminary results show that infection with an H1N1 strain of the influenza virus leads to an increase in potassium channel expression as well as the release of many pro-inflammatory cytokines.
These early findings suggest that potassium channels may be potential targets for drug therapy in treating severe cases of influenza virus infection, says Loewen.
Taryn Waugh of Saskatoon, Sask., is a second-year veterinary student who was part of the WCVM's Undergraduate Summer Research and Leadership program in 2014. Taryn's story is part of a series of articles written by WCVM summer research students.
