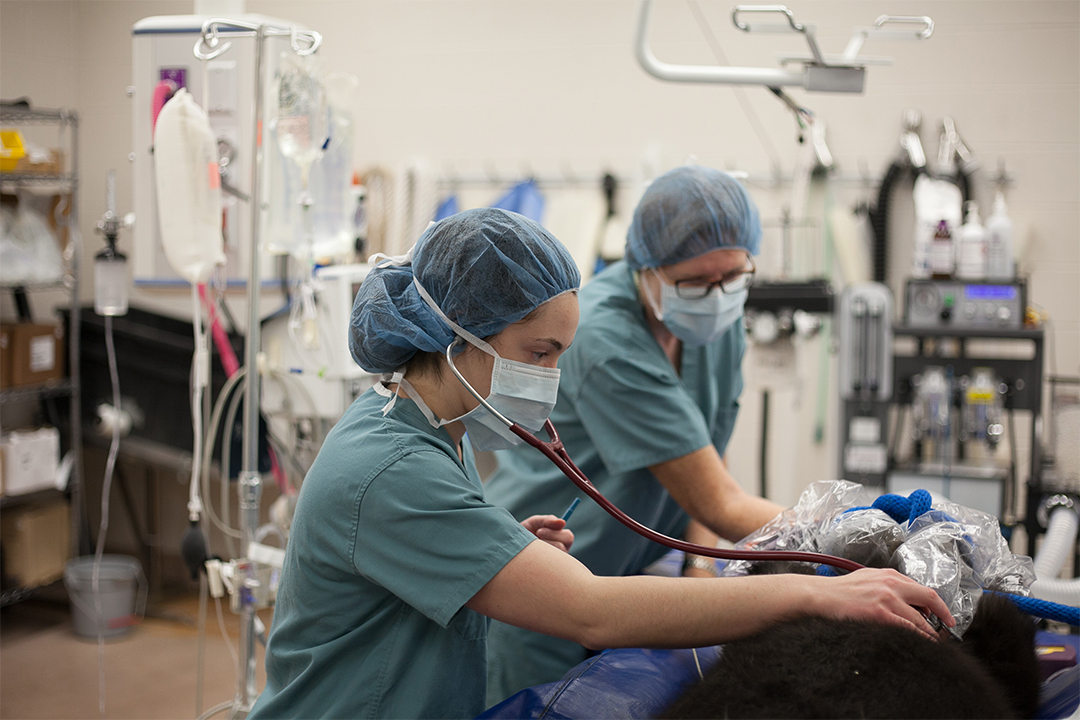
Anesthesiologists essential to patient care
Rounds, where each patient's plan for the day is reviewed, begin at 8 a.m. The room is full of scrubs and sneakers and coffees.
By Christina WeeseA dozen fourth-year veterinary students at the Western College of Veterinary Medicine (WCVM) are taking their clinical rotation through anesthesia for four weeks; each has a case plan written up that is presented to the panel of three board-certified anesthesiologists — Drs. Tanya Duke, Shannon Beazley and Rocio Fernandez-Parra.
Today's cases at the WCVM's Veterinary Medical Centre are varied. On the small animal side, several dogs are in for dental surgeries, while a canine patient is here with injuries related to a car accident that happened several months ago. Another dog with mobility issues is in for X-rays, a CT (computed tomography) scan and an MRI (magnetic resonance image) scan with possible surgery to follow. A pony in the VMC's Large Animal Clinic is also scheduled for surgery.
All plans go through several checks. Team members thoroughly discuss dosages of drugs and possible complications due to the patient's weight, condition and medications.
"Teamwork is imperative," says Duke, a professor of veterinary anesthesiology at the WCVM. "We rely on each other to double-check everything."
After rounds, veterinarians and students disperse to track down their patients in the veterinary medical centre.
Over in the equine ward, a clinical team brings in a small black pony — a colt — for cryptorchid surgery. Cryptorchidism is when one or both testicles don't descend from the body cavity, meaning the pony can't be gelded using the normal castration procedure. The surgeon will search inside for the animal's undescended testicle and then surgically remove it.
Dr. Duke and fourth-year student Simone Becker start readying the pony for anesthesia while the large animal surgical team and other students observe. With horses and other large animals, a definite protocol must be followed to bring them down safely — both for the animal and for the clinical team.
"Forty? Are you happy with 40 [beats per minute]?" Duke asks Becker, making sure she understands what the numbers mean as they monitor the pony's heart rate. Duke reviews signs of sedation in horses with the students and takes the opportunity to go over some possible drug interactions that they'll need to watch for. She also discusses what they'd be doing differently if they were taking the pony down for a routine castration out in the field.
The sedated pony is lifted onto a bright blue padded table and preparation for surgery begins. A team member clips the incision area while Duke and Becker affix an oxygen administration device to the pony's breathing tube.
"We keep him down with injectables [drugs] during prep," explains Duke. "The gas anesthetic starts once he's taken into the surgical room."
 From here, it's a matter of time and numbers.
From here, it's a matter of time and numbers.
"[It's] a whole bunch of constantly looking at stuff," says Duke. Until the electronic monitors come online, which can take a couple of minutes, the anesthesia team members manually monitor the patient's heart rate and breathing with a watch and a stethoscope.
Drug dosages are recorded on the pony's chart. Duke assists Becker in putting a nerve block (anesthetic drug that's injected directly near the nerve to block pain) in the animal's one descended testicle. Of course, they can't block the other testicle as its location is unknown.
When Duke and Becker are satisfied that they've done their job, the surgeon steps in. Duke begins to watch a long list of numbers: the heart's electrical activity on an ECG (electrocardiogram), arterial blood pressure, entitled carbon dioxide, oxygenation (the patient's 02 status) and respiratory rate. She also monitors the pony's temperature as animals can lose body heat or overheat while surgical procedures are happening.
These monitors, which are similar to the ones used in human hospitals, each cost between $25,000 and $35,000. As Duke explains, the most expensive part of the monitor measures how much anesthetic and oxygen is being breathed in and out by the patient. This gives the anesthesia team a much more accurate measurement than just watching the clinical signs to judge depth of anesthesia.
Part way through surgery, the colt's blood pressure increases as the surgeon removes the interior testicle, stimulating the pony's autonomic nervous system. Duke adjusts the colt's dosage upwards and monitors him, waiting for his blood pressure to come back down. When the surgeon removes the second testicle, which has been treated with the nerve block, there's no blood pressure fluctuation.
Duke discusses the pony's different reaction with Becker. "It's been proven to be worth doing the nerve blocks, where we can," she says, "and that's exactly why."
The surgery is successful, and the colt is readied for recovery. Over in the Small Animal Clinic's dentistry suite, Dr. Teresa Jacobsen is about to start a dental procedure on a small Shih Tzu dog. Anesthesia technician Kim Foster guides senior veterinary student Julie Hamilton in placing a tie so the animal's ventilator tube stays in place during surgery.
With her tools prepped, Jacobsen waits patiently as the anesthesia drugs start to work on her patient.
"Anesthesia is the team that smiles and nods and puts up with the last-minute requests from all the other teams," says Jacobsen with a laugh. "They get asked to squeeze things in a lot."
It's true – because animal patients can't sit still on their own, some form of sedation or anesthesia is needed for nearly all the medical imaging that happens in the veterinary medical centre. Radiographs are straightforward, but radiation therapy and MRIs require special circumstances.
In the VMC's pet radiation therapy centre, anesthesia technician Lindsey Fenez is monitoring a cat undergoing radiation therapy for a brain tumour. Several students, along with the centre's veterinary radiation oncologist and radiation technician, wait alongside her.
"You try to make everything perfect before leaving the room because once [radiation therapy] starts, you have to wait outside until it's done," explains Fenez. "Treatments only last about 10 minutes, though. If things go really wrong, we stop treatment and go back in to help the patient."
Across the room at the MRI machine, anesthesia technician Terry Osborne Cross is monitoring a Weimaraner dog that is undergoing spine imaging. She's joined by fourth-year veterinary students Alex Robinson and Luke Nickel as well as veterinary technologist Sharon Martin and Jin Huang, medical imaging technician.
The situation is a little different with MRI cases: imaging can take up to an hour and a half, but veterinary technologists can stop and start the machine when things need to be adjusted. The anesthesia equipment is located outside the imaging room, and patients are hooked up by long plastic tubes that run through a hole in the wall.
 Animals undergoing MRIs need to be immobilized, but because the procedure isn't painful, they don't need sedation for pain control. Depending on the patient, they're often breathing on their own and not hooked up to a ventilator. Patients are kept on the lightest dose of anesthetic needed to complete the procedure.
Animals undergoing MRIs need to be immobilized, but because the procedure isn't painful, they don't need sedation for pain control. Depending on the patient, they're often breathing on their own and not hooked up to a ventilator. Patients are kept on the lightest dose of anesthetic needed to complete the procedure.
As the MR imaging process begins, the Weimaraner starts to show some signs of movement. Osborne Cross calls one of the anesthesiologists, Dr. Shannon Beazley, to adjust the patient's dosage so the imaging can continue.
"We have very skilled anesthesia technicians," says Duke. "They are ‘in charge' of patients as they move around the hospital."
The technicians, who are all registered veterinary technologists (RVTs), are also responsible for making sure each patient's plan is carried out to the letter, and for letting the overseeing veterinarian know when something goes wrong.
"It takes two to three years to get technicians trained and comfortable in anesthesia," Duke explains. "A trained technician is an extremely valuable member of our team – we couldn't function without them."
It's now noon — the day shift is half over. Duke has another horse to prepare for surgery this afternoon, and will be on call in case of emergencies at night. Emergency trauma cases may need anesthesia for surgery, or the clinical team may need to induce a coma to give a severely ill patient's body time to heal. The patients may be on a ventilator and need constant monitoring to ensure blood pressure, heart rate and breathing all stay on board.
One such case was Angus, an Alaskan malamute puppy that was run over by a vehicle in 2016. He was on a ventilator for five days – the longest that the anesthesia team had successfully kept a canine patient on a ventilator at the VMC. Duke and Beazley — along with anesthesia residents Drs. Teela Jones and Valentina Carrozzo — were at Angus' side for much of that time.
But with luck, there will be no emergencies tonight — just an early start tomorrow, a round of patients and another day as part of the WCVM veterinary anesthesiology team.
